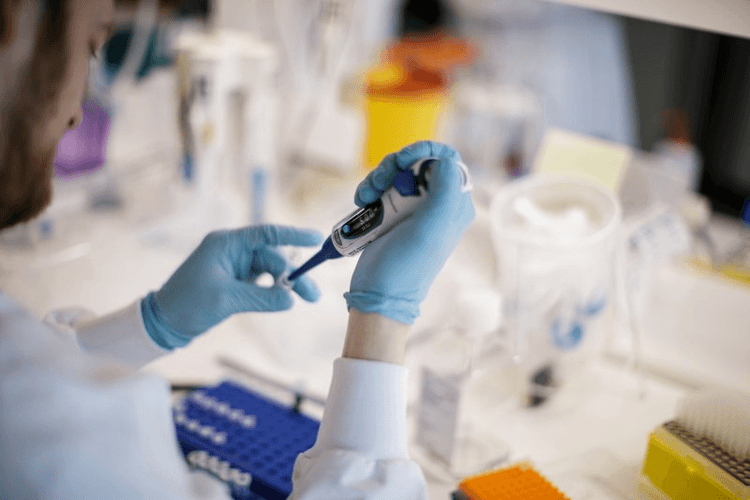
As people around the world continue efforts to flatten the curve and stop the rapid spread of the COVID-19 pandemic, questions are arising about the realistic expectations we should have for a vaccine.
Will they be distributed to everyone? How are we going to manufacture them rapidly enough to meet mass demands?
These questions don’t necessarily have easy answers, but back in April earlier this year Thomas Insights spoke to members of the team at JSI, an organization of healthcare/health systems consultants and researchers who have been working to strengthen both domestic and international health systems for a medical emergency just like this one.
We are republishing this interview in light of rapid progress being made to develop a vaccine for COVID-19.
In the Q&A below, Penelope Riseborough, JSI’s director of communications, Lora Shimp, technical director at JSI’s Immunization Center, and Wendy Prosser, the senior technical adviser for JSI’s Immunization Center, shared how the COVID-19 vaccine will be mass-produced and distributed when finally ready for public use.
Q&A with Immunization Experts at JSI
Thomas Insights (TI): What is JSI currently working on to aid healthcare professionals in the fight against the COVID-19 pandemic?
Penelope Riseborough (PR): "For JSI, at large, it really depends on the country; the work we’re doing is quite different in different places. We do a lot of work in the U.S. In New Hampshire, [for example,] we’re supporting the Department of Public Health and putting out COVID messaging and providing other support. We do a lot of work around mental health and substance abuse issues there, so we are also looking at what COVID means for people suffering from mental health issues or substance abuse.
We’re doing a lot of work around helping governments procure the supplies they need, whether it’s personal protective equipment and other materials for supply chain procurements.”
TI: What are some of the challenges you’re observing in vaccine development specific to COVID-19?
Lora Shimp (LS): "The challenge is that oftentimes vaccine production processes take years; even the clinical trial processes will take a minimum of six to nine months, or often longer.When a vaccine is developed for a particular virus that has longer-term implications, part of the process is considering the epidemiology and disease burden, assessing the demand for it, and finding out what the market is.
For COVID-19, everybody globally is looking for this vaccine.
Some of the different vaccines in production may be focusing more on the domestic market whereas others might be looking for an international market where they can quickly have the vaccine available, not only for their local consumption but also to share with the global community. But it’s going to have to go through a regulatory process within its own country for domestic manufacturing before it can go then through the WHO prequalification process… for global distribution of the vaccine and its use in other countries.
As you’ve heard Dr. Fauci describe in some of the WHO communications… they have worked on these types of pandemic-type vaccines before, like SARS and H1N1. So there are lessons they can learn from SARS and H1N1, for example.
But what COVID-19 is showing us is that there is going to be an extreme demand upfront, which is unlike what we’ve seen for most of the other vaccines.”
TI: Once researchers have developed a vaccine that’s deemed safe for the public, how are manufacturers going to scale up production rapidly enough to produce it in the quantities needed to have a substantial global impact?
LS: "You can’t mass-produce it right away because first, you want to know that your product is sound and meets all the criteria. Once they’re into phase two and three clinical trials, if they feel that their product is strong, some of the manufacturers now might already be preparing guidelines… so that as soon as they are close to being able to get approval, they can immediately produce.
In many cases, the manufacturers will do their market-shaping while they are awaiting the approvals from the regulatory authority. Or they’ll do the market-shaping, but they won’t be able to do mass production until they have the approval.
Given the urgent demand, many manufacturers are probably already starting to think about this. They will be considering how quickly they can produce the vaccine and if they have the lines of production ready so that they can basically hit the "go” button on mass-producing it as soon as they have passed the levels of approvals.
For some vaccine manufacturers, it will be challenging. They can’t immediately build production lines or just stop the production on one vaccine and immediately convert that over to another vaccine, because the process might be different.
For example, one might be a freeze-dried vaccine [while] the other might be a liquid vaccine, so they’re not interchangeable. But you do need to make sure that your product line is ready for production, has passed [necessary] inspections through the national regulatory authority, and then [determine] how quickly can it be mass produced.”
TI: Once the vaccine is produced, it will have to be distributed very rapidly. How do vaccine manufacturers’ supply chains differ from others?
Wendy Prosser (WP): "Most vaccines require a cold chain, which needs to be between two and eight degrees Celsius for the vaccine to stay potent and maintain quality. We don’t know what the COVID vaccine will look like and what it will require. It might not need a syringe. It might use some microarray patches or different ways to administer the vaccine, but most likely it will require a cold chain.
Most places at the national level will have cold trucks, like the refrigerated trucks that we see around here, that will deliver to some regional level or the state level. From there, down to the health facility level, most vaccines are delivered with 4×4 trucks in cold boxes, which are not very reliable in terms of maintaining temperature – which could reduce potency.
The exposure to heat or to freezing is kind of an accumulative thing for vaccines. If it goes up to 15 degrees Celsius for four hours today but then back to normal, [maintains a] perfect temperature for a long time, and then it gets exposed to heat again several days later, all of that accumulates.
The cold chain equipment is just one part within an overall system, and if that system is not strong enough to support the vaccine distribution, then that’s when you’re going to have issues with the vaccine maybe not being as potent or of the best quality.”
TI: How is the virus impacting researchers’ vaccine development and testing efforts?
WP: "From the manufacturer on, it’s mostly going through UNICEF through airplane delivery for efficiency. One thing that we’re seeing in many countries that we’re supporting is that a lot of the flights are canceled, so vaccine deliveries are being canceled, delayed, or need special approval to receive in-country.
We’re already seeing some changes with the current vaccine supply chain; trucks that could be used for vaccine delivery are now being used for delivering PPE or healthcare workers to different areas for outreach or to track those folks who have been exposed to the virus.
So it’s addressing the immediate impact of COVID, but also thinking long-term about when the COVID vaccine is available and how supply chains can be more resilient to be able to incorporate those vaccines into a regular, strong supply chain.
There is definitely a lot of attention these days on strengthening the supply chain within countries, but there are a lot of issues and the entire system needs to be strengthened. Little by little, countries are getting there, but now this pandemic is reshuffling priorities and readjusting those systems that have been working to get us stronger; it’s kind of setting everything back.”
TI: How are UNICEF and other health organizations going to determine which consumers are prioritized for vaccinations?
LS: "That is a very good question and a very complicated question. Obviously the challenge that non-manufacturing countries face is gaining access to the vaccine once it’s available and approved for an international market. So the countries that have vaccine-manufacturing capability are at an advantage — e.g. the United States, Europe, and others.
But if you’re a country that may not have the manufacturing capability for this vaccine, you won’t be the top priority. There will be a prioritization for the domestic market, having a vaccine available internationally, as well as vaccine development technology transfer. On an individual level, preference will most likely be to health workers where there is an upswing of the COVID curve so that they can quell additional transmission.
If a vaccine, hypothetically, becomes available next April, odds are they may not prioritize a country that’s on the down curve as much as they might prioritize a country that is just now starting to see cases because there’s potentially a buildup of immunity in the country that has gone through the epidemic. But, of course, that’s where the antibody testing is coming in. Can we say that you can’t get reinfected? We don’t know.
It’s similar to big negotiations that are happening around PPE and test kits. The vaccine will fall to that same competition. It will not be mass-produced fast enough to meet global needs all at once.”
TI: We’re seeing a lot of manufacturers step up to repurpose their facilities to help meet mass demands for supplies. Is there any opportunity for that in this supply chain?
WP: "It might be two-fold. One, from the manufacturer’s perspective, and then two, with in-country supply chains, it could be an opportunity for governments to rethink supply chains and figure out the best use for available trucks — the cold boxes, the cold chain equipment, how to best utilize that for all cold chain products, including a new vaccine coming in.
I think it’s a great opportunity for manufacturers to think about the different types of administration of the vaccine that is available. Lora can talk a lot about this new potential microarray patch that would be easier to administer. So that is on the pipeline.”
LS: "One thing that they’ve been looking at globally in immunization is being able to manufacture stable vaccines that do not require the cold chain and that can be administered more easily than the current use of a syringe and needle or even some sort of dropper. The microarray patch and other technologies being considered are ways that they’re trying to get vaccines more accessible where they could be administered by non-health people, whereas vaccines require a syringe and needle and therefore require someone who is qualified to give injections.
You wouldn’t need that necessarily with a microarray patch, as we’ve seen with some of the administration of oral vaccines like OPV. Someone who is not a trained nurse can give a polio vaccine because it’s just two drops. So that’s what they’re looking at potentially for some of these vaccines – administration through a technology that doesn’t require as intensive a cold chain or distribution process.”
Thomas is working with state and federal government offices to mobilize manufacturers who can produce COVID-19-critical products and supplies. If you already manufacture or can rapidly pivot to manufacture these products, please complete this form. If you are a hospital or other group operating on the frontlines of COVID-19 with an open P.O. to fulfill critical COVID-19-related product/service needs,click here.